Imaging Core Lab Services
WCG’s full-service medical imaging core lab provides comprehensive clinical trial imaging services to pharmaceutical, biotechnology and medical device companies across all therapeutic areas.
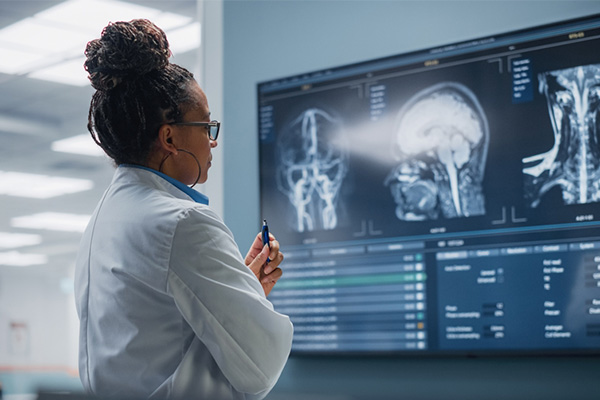
Comprehensive clinical trial imaging solutions
WCG Imaging is a full-service medical imaging core lab that supports pharmaceutical, biotechnology and medical device companies in conducting drug and medical device clinical trials.
We are also the world leader in conducting Artificial Intelligence (AI) / Computer Assisted Detection (CAD) clinical trials.
With our team of more than 600 board-certified and fellowship-trained physicians, WCG Imaging’s team has sub-specialization in all therapeutic areas, including Oncology, Cardiology, CNS, Gastroenterology, Musculoskeletal and Ophthalmology.
Board-certified, fellowship-trained physicians
ISO quality management system certifications
Imaging sites supported in 75 countries
Explore our Imaging Core Lab solutions:
Study Management
Our teams specialize in providing imaging core lab services in support of Phase I-IV Clinical Trials and Class I, II and III Medical Device Trials.
Our Project Managers are experts in study management and have proven records of managing international clinical trials across all therapeutic areas and indications.
We manage all aspects of imaging in clinical trials and ensure to guide it towards success.
Site Management
We specialize in managing international imaging sites participating in Phase I-IV Clinical Trials and Class I, II and III Medical Device Trials.
We currently support over 4,000 imaging sites in 75 countries, and we have extensive experience in qualifying and training imaging sites participating in clinical trials. We manage all clinical trial imaging sites and ensure that all sites are qualified, trained, and able to acquire and submit images as per the image acquisition protocol.
We ensure quality by monitoring all sites throughout the entire trial and quality control each and every timepoint immediately upon receipt to ensure the best possible imaging throughout the entire clinical trial.
Imaging Charter
At WCG Imaging, our team of more than 600 board-certified and fellowship-trained physicians, are experts in all therapeutic areas.
Our team has expertise in Oncology, Cardiology, Central Nervous System, Gastroenterology, Musculoskeletal and Ophthalmology and their indications. This expertise allows us to develop a sophisticated and optimized Imaging Charter with the appropriate review criteria.
At WCG Imaging, we ensure all of our reviewers are experienced, appropriately trained and have the expertise needed to ensure quality assessments of even the most complex of indications.
Image Acquisition Protocol
We recognize it is essential to ensure the correct acquisition of each participant’s imaging timepoint.
Our ISO certified processes ensure that the processing of participant images received from sites is meticulously planned, implemented and monitored for success.
Whether the images received are in support of a drug, medical device, or artificial intelligence (AI) clinical trial, our team has the expertise and experience to ensure quality and compliance of every participant scan.
Case Review
Our team consists of more than 600 full time and consulting board-certified, fellowship-trained physicians and key opinion leaders (KOLs) with sub-specialization in all therapeutic areas.
Using our ISO certified process, we plan, implement and monitor case reviews meticulously to ensure success. All of our reviewers are experienced, appropriately trained and have the expertise needed to ensure quality assessments of even the most complex of indications.
Whether the review is in support of a Phase I-IV clinical trial or in support of a Class I, II or III trial to study a medical device, our physicians have the expertise and experience to provide comprehensive services to pharmaceutical, biotechnology and medical device companies worldwide.
Data Management
Our technology allows us to provide robust data management and accommodate even the most specialized clinical and medical device trials.
Our data management team ensures that the case report, database and data exports are designed and configured optimally to ensure the data is acquired, validated, stored, protected, and processed as expected to ensure the accessibility, reliability, and timeliness of the data.
In addition to having one of the most comprehensive and sophisticated quality management systems, and leading the industry with 5 ISO certifications, our data management team also complies Good Automated Manufacturing Practice (GAMP®5).
Who We Serve
Pharmaceutical/Biotechnology
At WCG Imaging, our team consists of more than 600 board-certified, fellowship-trained physicians and key opinion leaders (KOLs) with sub-specialization in all therapeutic areas.
Our therapeutic expertise includes, but is not limited to Oncology, Cardiology, Central Nervous System, Gastroenterology, Musculoskeletal and Ophthalmology.

Medical Device
The WCG Imaging team has extensive experience in providing imaging core lab services in support of Class I, II and III Medical Device Trials.
WCG Imaging is the only ISO 13485 certified imaging core lab specifically certified to provide quality imaging core lab services for Medical Device clinical trials. WCG Imaging’s medical device certification was granted by the British Standards Institute (BSI), one of the world’s largest certification bodies.
Our fellowship trained physicians are responsible for a broad range of assessments and evaluations of medical devices across the range of therapeutic areas and are experts in protocol design and in the selection and the utilization of imaging modalities that are best oriented towards the placement, assessment and evaluation of various medical devices.

Artificial Intelligence Software (AI/CAD)
WCG Imaging is the world leader in conducting multi-case multi-reader studies to evaluate Artificial Intelligence (AI) and Computer Assisted Detection (CAD) systems.
We provide the most efficient means for Sponsors to conduct trials to assess the clinical performance of their AI/CAD software and obtain FDA clearance.
WCG Imaging is selected due to our:
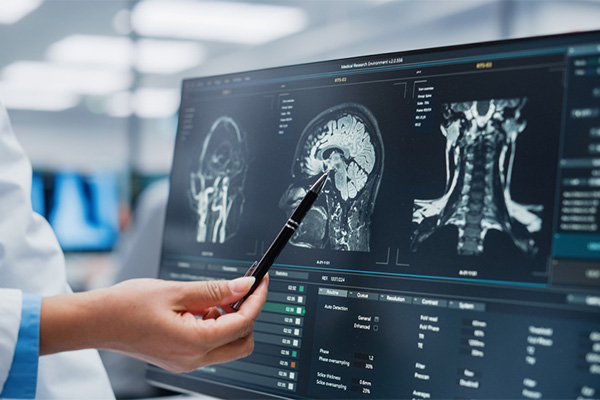
- Extensive experience & expertise in large AI trials
- Multiple successful FDA Inspections with zero 483
- Proven success with multiple FDA medical device clearances
- ISO Certified quality management system
- ISO 13485 certification specifically for medical devices
- Certified by the British Standards Institute
- Routinely manage 6,000-20,000 case reviews
ISO Certified Quality Management System
ISO Certified Imaging Core Lab
WCG Imaging has one of the most comprehensive and sophisticated quality management systems in the industry:
- Only imaging core lab in the world to hold three ISO quality management system certifications specifically for providing imaging core lab services on clinical trials.
- Inspected by the FDA with Zero 483s.
- Our quality management system is certified by the British Standards Institute (BSI).
Quality Management System
Unique in the industry, our quality management system is certified to ISO 9001, ISO 13485, and ISO 27001 by the British Standards Institute (BSI). Our certifications are specifically for providing imaging core lab services on clinical trials.
In addition to our team, technology and therapeutic expertise, our ISO-certified quality management system also provides Sponsors with high confidence in our abilities as a leading medical imaging core lab.

ISO 9001
Quality Management
IS0 13485
Medical Device Quality Management
ISO 27001
Information Security Management
Explore our therapeutic expertise:
Our Cardiothoracic Imaging Division has extensive experience in Cardiothoracic imaging in clinical trials, supporting Phase I-IV trials and medical device trials.
Our cardiologists and radiologists are fellowship-trained to provide the highest level of expertise in the evaluation of thoracic and cardiovascular diseases.
Our cardiothoracic team are accomplished researchers and educators, and several are internationally-recognized experts in cardiothoracic imaging serving in prominent roles within the Radiological Society of North America (RSNA), American Roentgen Ray Society (ARRS), Society of Thoracic Radiology (STR), Fleischner Society, American Board of Radiology (ABR), and American College of Radiology (ACR).
Cardiothoracic Imaging Expertise
- Acute and Chronic Heart Failure
- Acute Coronary Syndromes
- Aneurysms
- Asthma
- Bronchitis
- Carotid Artery Disease
- Congestive Heart Failure
- COPD
- Coronary Artery Calcium Scoring
- Coronary Artery Disease
- Cystic Fibrosis
- Deep Vein Thrombosis
- Diabetes
- Emphysema
- Interstitial Lung Disease
- Left Ventricular Dysfunction
- Mediastinal Disease
- Myocardial Infarction
- Obesity
- Peripheral Vascular Disease
- Pleural Disease
- Pneumonia
- Pulmonary Arterial Hypertension
- Pulmonary Embolus
- Pulmonary Tumors
- Sickle Cell Disease
- Valvular Disease
- Venous Thromboembolic Disease
Cardiothoracic Modality Expertise
- Angiography
- Cardiac CTA
- Cardiac MRI
- Chest Radiography
- CT, QCT, PET/CT
- CR/DR
- DXA
- 2D and 3D Echocardiography
- Electrocardiograms (ECG)
- MRA, MRI, MRE, Adenosine Stress MRI
- MUGA
- Myocardial Strain imaging
- Nuclear imaging
- Positron emission tomography (PET)
- Speckle tracking
- Thoracic Computed Tomography (CT)
- Thoracic High-Resolution CT (HRCT)
- Thoracic MRI
- Ultrasound
- Vascular CTA
- Vascular MRI
As an Imaging Core Lab, the WCG Imaging team has extensive experience in providing neuroradiology imaging services in support of Phase I-IV Clinical Trials and Medical Device Trials.
Our team of board-certified fellowship-trained neuroradiologists specializes in all brain and spine pathology with broad experience and expertise in neuroradiology imaging using MRI, Volumetric MRI, CT, diagnostic and interventional angiographic procedures, as well as PET imaging using novel CNS markers.
Neuroradiology Imaging Expertise
Our neuroradiology team consists of board-certified, fellowship-trained neuroradiologists with expertise in the full spectrum of brain and spine disease processes.
Modality expertise including;
- Catheter Angiography
- CT & CTA, including CT perfusion
- Diffusion tensor imaging
- MRI & MRA, including MR perfusion
- Volumetric MRI
- Nuclear imaging, including FDG PET
- SPECT
- Ultrasound, including transcranial doppler
Neuroradiology Imaging Indications
- Alzheimer’s Disease
- Aneurysm and vascular malformations
- Brain Tumors
- Cerebrovascular disease
- Epilepsy
- Huntington’s disease
- Multiple Sclerosis
- Neurointerventional devices
- Parkinson’s, including dyskinesia’s
- Polyneuropathies
- Schizophrenia
- Spinal degenerative diseases
- Spinal cord injury
- Stroke
- Traumatic Brain Injury
- Tumors
The WCG Imaging team has extensive experience in providing services in support of Phase I-IV Clinical Trials and Medical Device Trials involving gastrointestinal imaging.
Our board-certified gastroenterologists have an in depth understanding of the evaluation, prognosis, progression and treatment of GI related disorders. We also have further expertise and capabilities in interventional treatment techniques.
We are experts in the intervention of intestinal disorders including, but not limited to gastric, small bowel and colonic pathology, physiology and function.
We are able to guide the performance and radiographic interpretation of the entire digestive tract, including the pharynx, esophagus, stomach, duodenum, small intestine, colon and biliary system as well as all accessory organs to the alimentary canal.
Gastrointestinal Imaging Expertise
Our team of board-certified, fellowship-trained body and thorax radiologists review 500,000 body and thorax related images annually that encompass the full endocrine system.
Our radiologists are experienced in imaging of organ specific endocrine disorders as well as multiple endocrine syndromes and neoplasia.
Modality expertise including:
- CT including novel techniques
- High Resolution CT imaging and low dose techniques
- MRI
- Nuclear imaging with quantitative techniques
Expertise across all Indications
- Constipation
- Chronic diarrhea
- Crohn’s disease
- Gastro-esophageal reflux
- Inflammatory bowel disease
- Interstitial Cystitis
- Irritable bowel syndrome (IBS)
- Kidney Stones
- Neurogenic Bladder
- Pelvic Inflammatory Disease
- Prolapsed Uterus
- Short Bowel Syndrome
- Ulcerative colitis
- Ulcers – Gastric/Duodenal/H. Pylori
- Urinary Incontinence
- Diabetes and Diabetic sequelae
As an Imaging Core Lab, our team has extensive experience in providing services in support of Phase I-IV Clinical Trials and Medical Device Trials involving Musculoskeletal imaging.
Our expertise includes but is not limited to the full complement of joint and spine disease processes, musculoskeletal interventions including pain management and device.
Our multiple modality expertise in musculoskeletal imaging includes, but is not limited to, ultrasound, nuclear imaging, DXA, MR, and CT including novel techniques such as QCT, T2 Cartilage imaging, MARS imaging and kinetic MRI.
Musculoskeletal Imaging Expertise
- Board-certified, fellowship trained musculoskeletal radiologists
- Expertise including but not limited to the full complement joint and spine disease processes
- Expertise in Musculoskeletal imaging
Multiple modality expertise:
- CT
- DXA
- Kinetic MRI
- MARs imaging
- MRI
- Nuclear imaging
- QCT
- T2 Cartilage imaging
- Ultrasound
- X-Ray
Musculoskeletal Indications
- Ankylosing Spondylitis
- Arthritis
- Bone Age
- Bone Density
- Bone Repair
- Bone Healing
- Inflammatory Arthritis
- Psoriatic Arthritis
- Osteoarthritis
- Osteoporosis
- Orthopedic implants
- Muscular dystrophy
- Novel biologics
- Real time spinal motion
- Real time spinal kinetics
- Rheumatoid Arthritis
- Spinal muscular atrophy
As an Imaging Core Lab, our team has extensive experience in providing services in support of Phase I-IV Clinical Trials and Medical Device Trials involving Cancer.
Oncology Imaging Expertise
The oncology team includes board-certified, fellowship-trained radiologists focused in oncology. The team’s expertise includes the full spectrum of oncology imaging and assessments for all indications.
Multiple Criteria expertise:
- BIRADs (Breast)
- Cheson
- Choi
- Deauville
- irRC
- irRECIST & Immuno-Oncology
- LI-RADS (Liver)
- Lugano
- Macdonald
- mRECIST
- PCWG2
- PERCIST
- PI-RADS (Prostate)
- Rano
- RECIST
- TI-RADS (Thyroid)
Multiple modality expertise:
- CT including multi-slice
- MRI including DCEMRI and Novel techniques,
- PET/CT and Nuclear Imaging
Oncology Imaging Indications
- Breast
- Cervical
- Chronic Lymphocytic Leukemia
- Colorectal Cancer
- CNS/Head and Neck
- Gastrointestinal Cancers
- Hepatocellular
- Leiomyosarcoma/Liposarcoma
- Liver
- Lung
- Lymphoma
- Melanoma
- Ovarian
- Pancreas
- Prostate
- Renal Cancers
- Thyroid
Our team has experience in providing services in support of Phase I-IV ophthalmology clinical trials.
Our team consists of board-certified ophthalmologists and our expertise includes the full spectrum of ophthalmology imaging and assessments.
Oncology Imaging Expertise
- Adaptive Optics (AO) retinal imaging
- Best Corrected Visual Acuity (BCVA)
- Electroretinogram (ERG)
- Full Field Stimulus Testing (FST)
- Intra Ocular Pressure (IOP)
- Near infrared AF imaging
- Optical Coherence Tomography (OCT)
- Visual Field Assessments
Ophthalmology Imaging Indications
- Diabetic retinopathy
- Epiretinal membrane
- Macular hole
- Macular degeneration
- Retinal tear
- Retinal detachment
- Retinitis pigmentosa
- Spinal muscular atrophy
Contact WCG Imaging to discuss your trial’s imaging needs
We have the team, therapeutic expertise, technology, and ISO-certified quality management systems to provide imaging core lab services to our clients worldwide. Complete the form to get started.


